Peripheral Angiography ( for PDA)
Peripheral Angiography ( for PDA)
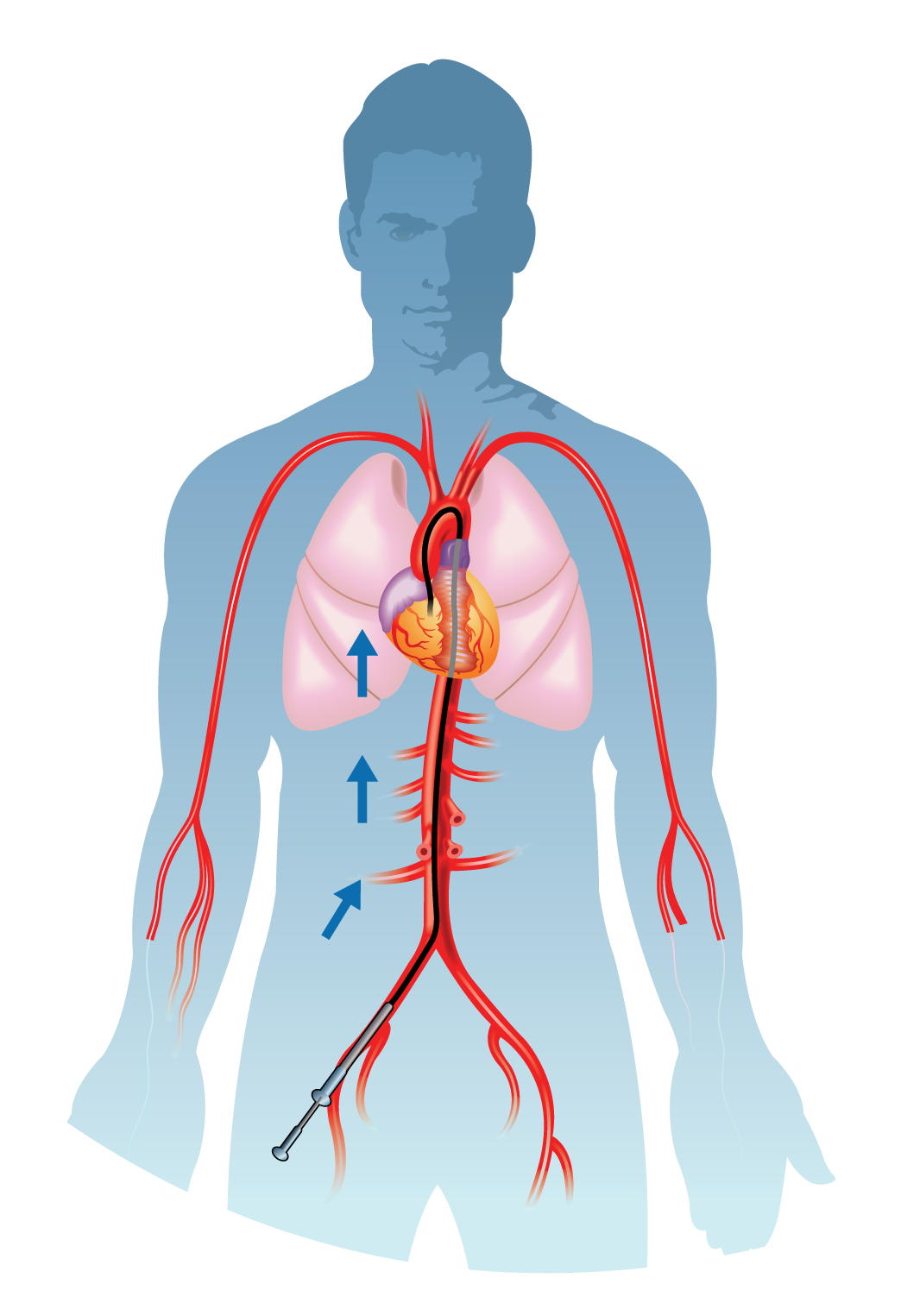
Peripheral Angiography for Patent Ductus Arteriosus (PDA) is a diagnostic procedure designed to assess and visualize the blood vessels supplying the periphery of the body, with a specific focus on the ductus arteriosus—a vital fetal blood vessel that connects the pulmonary artery to the aorta. In cases where the ductus arteriosus fails to close after birth, termed Patent Ductus Arteriosus (PDA), peripheral angiography becomes a crucial tool for evaluation.
During the procedure, a catheter is threaded through blood vessels, often starting in the groin area, and guided to the site of interest. Contrast dye is injected through the catheter, allowing X-ray visualization of the blood vessels and highlighting any abnormalities related to the PDA. The images obtained provide detailed information about the size, location, and blood flow through the patent ductus arteriosus.
Peripheral Angiography aids healthcare providers in determining the most appropriate treatment strategy for PDA. While some PDAs may close on their own, others may require intervention. Closure devices, either inserted through a catheter or through open-heart surgery, are used to seal the PDA, preventing abnormal blood flow and promoting normal heart function.
Post-angiography, patients are monitored for potential complications, with most individuals experiencing a relatively short recovery period. The insights gained from Peripheral Angiography play a crucial role in personalized treatment decisions, ensuring optimal care for individuals with Patent Ductus Arteriosus and contributing to improved long-term cardiovascular health and well-being.
Approach
For everyday care or life-changing care you can count on our doctors.
Experts
You can count on us to keep you and your loved ones safe and healthy.
Technology
Cardiac rehabilitation (CR) can slow or reverse the nurse progression.
Facilities
We use a team approach to providing health care, and involve the patient.
Peripheral Angiography ( for PDA)
It seems like you may be referring to a scenario where there are restrictions or limitations related to coronary angioplasty. If you have specific details or concerns in mind, please provide more information so I can offer a more accurate response.
Coronary angioplasty, or percutaneous coronary intervention (PCI), involves dilating narrowed coronary arteries. A catheter with a deflated balloon is advanced to the blockage site. Upon reaching the narrowed segment, the balloon is inflated, compressing the plaque and widening the artery. This dilation restores blood flow, relieving symptoms and improving overall cardiac function.
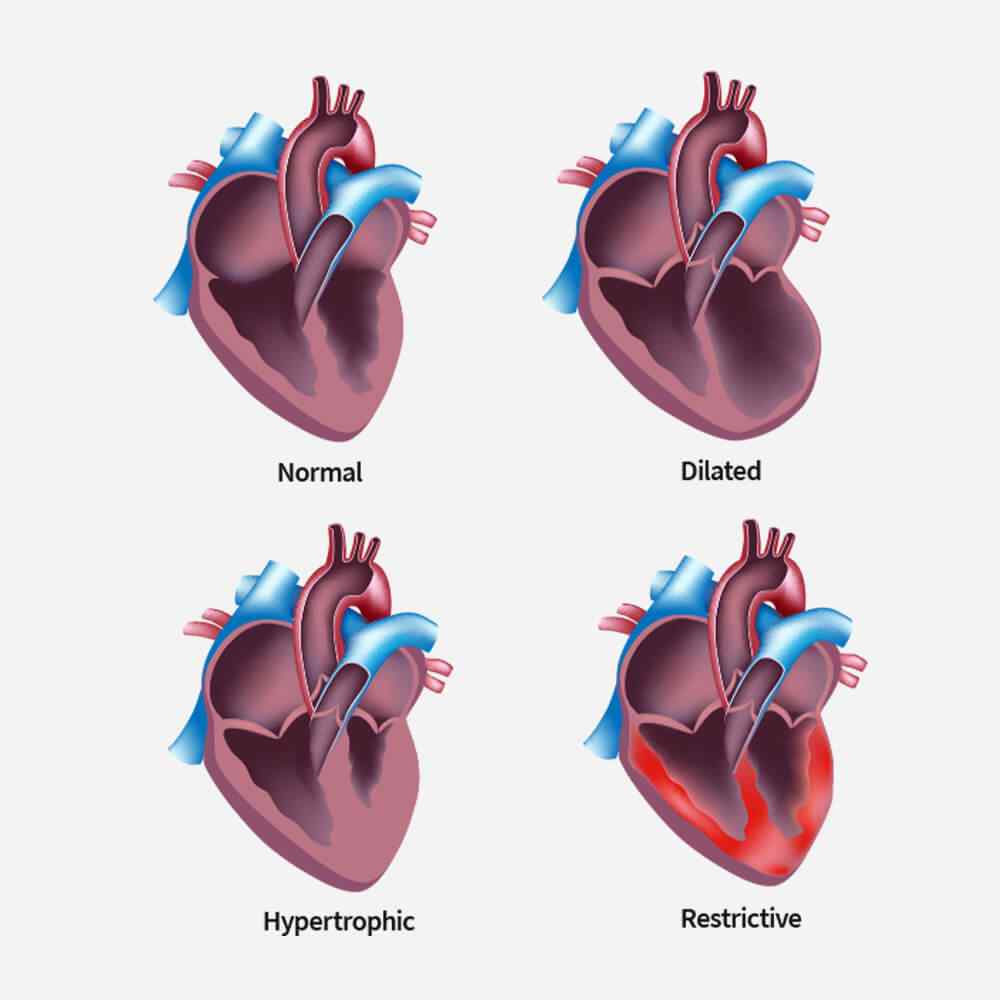
Coronary angioplasty is a procedure primarily used to address coronary artery blockages. However, for hypertrophic conditions like hypertrophic cardiomyopathy (HCM), angioplasty may not be the first-line treatment. HCM involves thickening of the heart muscle and is typically managed through medications, lifestyle changes, or in severe cases, surgery. Angioplasty isn’t a standard approach for hypertrophic conditions. Always consult with a healthcare professional for personalized advice.
Coronary angioplasty primarily addresses blockages in coronary arteries supplying blood to the heart muscle. It isn’t typically performed in the right ventricle, which is a chamber of the heart responsible for pumping blood to the lungs. Procedures involving the right ventricle, such as right heart catheterization, differ and are usually conducted for specific diagnostic purposes or conditions affecting that particular heart chamber. Always consult with a healthcare professional for personalized medical advice.
Related TreatmentPeripheral Angiography ( for PDA)
Peripheral Angiography is a diagnostic procedure typically used to assess blood vessels, but its application to Patent Ductus Arteriosus (PDA) might be an error, as PDA involves a connection between the aorta and pulmonary artery, not peripheral vessels.
