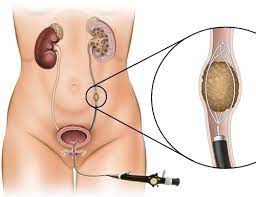
Kidney Stone Surgery
Indications:
Surgery for kidney stones is typically considered when the stones are large, causing severe pain, obstructing urine flow, leading to recurrent urinary tract infections, or causing kidney damage. In some cases, the type of kidney stone or the patient’s medical history may also influence the decision to pursue surgical intervention.
Preparation:
- Evaluation: Before surgery, the healthcare provider will conduct a thorough evaluation, which may include imaging tests (such as CT scans or ultrasound) to assess the size, location, and composition of the kidney stones.
- Medical History Review: The healthcare provider will review the patient’s medical history and any previous treatments for kidney stones.
- Preoperative Instructions: Patients will receive specific preoperative instructions, which may include guidelines for fasting, medication adjustments, and other preparatory measures.
Surgical Procedures:
Extracorporeal Shock Wave Lithotripsy (ESWL): This non-invasive procedure uses shock waves to break up kidney stones into smaller fragments that can be passed out in the urine. ESWL is typically suitable for smaller stones located in the kidney or upper ureter.
- Ureteroscopy (URS): A thin, flexible scope is passed through the urethra and bladder into the ureter and kidney to directly visualize and remove or fragment stones using laser or other instruments.
- Percutaneous Nephrolithotomy (PCNL): In this procedure, a small incision is made in the patient’s back, and a nephroscope is used to remove or break up larger kidney stones located in the kidney through direct access.
Postoperative care:
Follow-up Appointments: Patients will have follow-up appointments to monitor their recovery, assess any potential complications, and discuss strategies to prevent future kidney stones.
- Medication: Depending on the type of kidney stone and the patient’s medical history, the healthcare provider may prescribe medications to prevent the formation of new stones.
- Dietary Recommendations: Dietary modifications, such as adjusting fluid intake and specific dietary restrictions, may be recommended to reduce the risk of recurrent kidney stones.
Benefits:
Risks: Potential risks of kidney stone surgery include bleeding, infection, damage to surrounding structures, and the need for additional procedures.
Benefits: Surgery for kidney stones aims to alleviate symptoms, remove or fragment stones, prevent complications, and improve urinary function.
Recovery and Alternatives:
Recovery:
Hospital Stay: Depending on the type of surgery and the patient’s specific situation, a hospital stay may be required for observation and postoperative care.
Pain Management: Patients will receive pain management strategies to relieve discomfort and manage postoperative pain.
Fluid Intake: Adequate fluid intake is essential to help flush out stone fragments and prevent dehydration.
Alternatives:
In some cases, smaller kidney stones may pass naturally without the need for surgical intervention. Other treatment options, such as medication, dietary modifications, and procedures like ureteroscopy or extracorporeal shock wave lithotripsy, may be considered based on the specific characteristics of the kidney stones and the patient’s medical history.
The decision to pursue surgery for kidney stones should be made in consultation with a healthcare provider, taking into account the size, location, composition, and impact of the stones on the patient’s health and quality of life.
Follow-up:
After a laparoscopic splenectomy, patients typically require regular follow-up appointments with their healthcare provider to monitor their recovery, address any concerns, and assess immune function. The healthcare team may provide guidance on vaccinations and antibiotics to reduce the risk of infections. Periodic imaging studies and blood tests may be conducted to ensure the patient’s ongoing health and well-being.
It is important to emphasize that the overview of laparoscopic splenectomy treatment should be tailored to address the specific indications for the procedure and the individual’s unique circumstances. Patients are encouraged to actively engage with their healthcare team, ask questions, and seek the information necessary to make informed decisions about their care.